Ian CT TSE
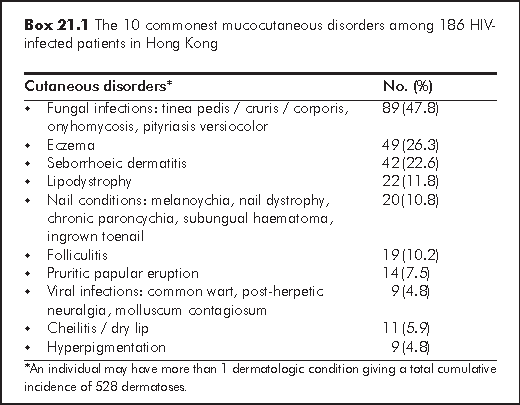
Skin disorders are commonly encountered in HIV-infected patients, and they may be the first manifestation of HIV disease. Up to 90% of HIV-infected persons suffer from skin diseases during their course of illness.1 In a local cross-sectional study of 186 HIV positive patients, 175 (94%) suffered from one or more cutaneous disorders.2 The most common skin disorder identified was fungal infection, followed by eczema and seborrhoeic dermatitis (Box 21.1). The spectrum of skin disorders depends on:
(a) immunologic stage, as reflected by CD4 count
(b) concurrent use of HAART
(c) pattern of endemic infections
In general, declining immunity is associated with increased number and severity of skin disorders.3 Skin lesions are more likely to have unusual appearance in advanced HIV infection.

The advent of HAART has changed the spectrum of skin disorders by improving host immunity, which in turn reduces the occurrence of Kaposi's sarcoma and some of the skin infections (Box 21.2).4 However, the restoration of immunity may cause flare-up of herpes zoster. HIV-infected patients are more likely than the general population to suffer from adverse drug reactions. HAART, with no exception, carries the risk in causing mucocutaneous adverse reactions (Box 21.3).5,6 One of the commonly encountered problems in HAART era is the protease inhibitor (PI)-induced lipodystrophy which is characterised by loss of buccal fat, thinning of extremities and buttocks, central adiposity ("crix-belly"), dorsocervical fat pad ("buffalo hump") and gynaecomastia.
Cutaneous manifestations may vary with one's geographic location. Penicilliosis, for example, is more common in South East Asia and Hong Kong than in the Western World.
Skin diseases of HIV-infected persons can be systematically classified by their pathogenesis (Box 21.4).2 Selected skin diseases are discussed in this chapter.
The drug history, morphology of primary lesion4 (Box 21.5) and CD4 count4,7 (Box 21.6) are important clues to skin diagnoses. In many cases, HIV-associated skin diseases can be easily recognised on clinical grounds, especially in the early HIV disease where clinical atypia is less frequent.
When diagnostic difficulty is encountered, skin biopsy should be considered for both histologic and microbiological evaluation. As HIV-infected persons frequently have more than one dermatosis, several biopsies may be necessary.





Skin diseases are rarely life-threatening, but many of them are life-ruining. While the lifespan is prolonged by the use of HAART, many HIV-infected patients are troubled by drug-induced facial lipoatrophy. Not only can there be cosmetic disfigurement, the intense pruritus due to eosinophilic folliculitis may severely impair the patients' quality-of-life. Therefore, management of these apparently minor conditions should not be overlooked.
In most cases, treatment modality of skin diseases in HIV-positive patients is similar to that in HIV-negative ones. However, prolonged high-dose systemic steroid should be used with caution because of the immunosuppressive effects. Although phototherapy can alleviate pruritus or improve psoriasis in HIV-infected patients, its use is hampered by its upregulation of HIV transcription.8
Acute seroconversion syndrome is very much like Epstein-Barr virus infection. The patient presents with fever, sore throat, cervical adenopathy and exanthem which occur in 70% of the cases.9 The exanthem is an erythematous maculopapular eruption that may become confluent. This eruption distributes over the trunk and sometimes the palms and soles resembling secondary syphilis. Oral and genital erosions have also been reported. The histology is non-specific. It shows mononuclear cell infiltrates in the upper dermis.
Cutaneous manifestation is an important clue of Penicilllium marneffei infection as it presents in more than 75% of the cases.10 The characteristic skin lesions of disseminated P. marneffei are umbilicated papules with or without central necrosis. Nevertheless, penicilliosis can manifest as ulcers, nodules, maculopapules, acneiform lesions or folliculitis. Wright, Giemsa or PAS stain demonstrates intracellular and extracellular yeast-like organisms that are spherical to elliptical shape. The basophilic organisms have clear transverse septa.
Bacillary angiomatosis is an infectious disease of skin and viscera characterised by angiomatous lesions. The causative agents are B. quintana and B. henselae. It is seen in patients with CD4 <100/μL and with history of cat scratch or bite. It presents as single or multiple red-purple nodules on the eyelids, mucosae, liver or spleen. Histology shows lobular capillary proliferation. Warthin-Starry stain demonstrates clumps of bacilli. It can be effectively eradicated by erythromycin, doxycline or minocycline.
Mycobacterial disease is caused primarily by Mycobacterium tuberculosis, M. avium intracellulare (MAI), and rarely by M. kansaii, M. fortuitum and others. The altered immunity in HIV disease may result in the absence of characteristic histology, such as caseating granuloma. An accurate diagnosis relies on the demonstration of acid fast bacilli or positive tissue culture.
The skin lesions of these mycobacterium species may take the form of nodules, plaques, papulonecrotic lesion, pustules, abscess or erythema nodosum. In practice, skin lesions of mycobacterial infection are rare even in the commonly encountered M. tuberculosis and MAI infection.
Infection with HSV is extremely common in HIV disease. It usually represents the reactivation of latent virus. The usual manifestations are orolabial vesicles, anogenital disease or herpetic whitlow. However, facial lesions manifested as folliculitis has been reported.11 In advanced HIV disease, HSV is more likely to be persistent and atypical in appearance: verrucous erosions, deep ulcers or large ulcer reaching 20 cm in diameter. Treatment response to acyclovir is often less marked than the immunocompetent individual. Continuous suppressive treatment with acyclovir 400 mg bid is considered for frequent relapses, such as >6x /year. Some clinicians prefer the use of valacyclovir or famciclovir because of improved pharmacokinetics and convenience of administration. For acyclovir-resistant HSV, intravenous foscarnet or cidofovir can be used.
Varicella zoster virus infection can occur at any stage of HIV disease. HIV infected children who develop chickenpox are more likely to suffer from complications such as pneumonia than non-HIV infected individuals. Herpes zoster is common in the early stage of HIV infection and may be the first clue of HIV infection in a young healthy adult. Clinical appearance of herpes zoster among HIV positive persons does not differ from those of HIV negative persons. However, multidermatomal lesions are more frequent in advanced HIV disease. Atypical features such as necrotic punched-out ulcers or hyperkeratotic ulcerated nodules have been reported. Treatment of uncomplicated herpes zoster by oral acyclovir 800 mg 5x/day is usually effective. In disseminated VZV infection, intravenous acyclovir (10 mg/kg q8hr for 7-10 days) is preferable due to its improved bioavailability. Interestingly, herpes zoster may develop as immune reconstitution syndrome when CD4 count rises to 300/μL.
It is caused by pox virus that selectively infects human epidermal cells. Lesions are usually multiple and have a predilection for the face and genitalia. Although the typical lesions are pearly papules with central umbilication, atypical lesions such as giant mollusca have been reported in advanced HIV disease. Molluscum contagiosum in HIV-infected patients is unlikely to resolve spontaneously and is notoriously difficult to treat. Treatment options include cryotherapy, curettage, excision and topical tretinoin. HAART makes the existing lesions more responsive to the above treatment.
Both verruca vulgaris and condylomata acuminata are common in HIV disease. There is an increased incidence of facial and intraoral warts. The extent of disease and the number of HPV types tends to increase as the CD4 count drops. In the anogenital area, condylomata acuminata may form large vegetating masses or may extend into the anal canal where squamous cell carcinoma may develop. Recent study suggests routine anal cytology to all HIV-infected men especially in those with low CD4. Similar to HIV-negative persons, the treatment goal in HIV positive persons is to remove the exophytic lesions. This can be achieved by podophyllotoxin, imiquimod, CO2 laser, curettage or surgical removal. Although topical cidofovir gel is not commercially available, its efficacy on the treatment of recalcitrant condylomata acuminata has been reported.12
Although systemic CMV infection is common in HIV-infected patients, mucocutaneous lesion is rare. The most common presentation is oral or perianal ulcer. Nonetheless, papulovesicular eruptions, purpura, nodules and verrucous lesions have been reported. The presence of CMV in the skin lesions does not necessarily indicate its pathogenic role. In many cases of mucocutaneous CMV, concomitant infectious agents such as HSV or mycobacteria were identified. These infectious agents alone could induce the aetiologic process. Furthermore, CMV has occurred in apparently healthy skin. Dauden et al believed that CMV does not play significant pathogenic role in most cases.13
Mucocutaneous candidiasis, usually caused by C. albican, is one of the most common mucocutaneous finding in HIV disease. It manifests as oral thrush, angular cheilitis, intertrigo, balanitis, paronychia, balanitis and vaginal thrush. Diagnosis is usually based on clinical ground. The presence of psuedohyphae in KOH preparation or wet mount confirms the diagnosis. Topical antifungal agent is usually adequate.
Tinea infections and onychomycosis are common in HIV disease. The features are generally similar to the non-HIV infected individual. Cutaneous fungal infections can mimic inflammatory dermatosis such as seborrhoeic dermatitis or psoriasis, but the asymmetry of lesion suggests a fungal aetiology.
Tinea unguium frequently associates with tinea pedis and produces sub-ungual hyperkeratosis, onycholysis and nail discoloration. "Proximal white subungual onychomycosis" is an unusual presentation and is more specific to HIV infection. Topical therapy is usually not effective. Terbinafine is highly efficacious for dermatophytic infection, but not predictably effective for nondermatophytic fungal infection. Terbinafine is given at 250 mg/day for 6 weeks (fingernail) or 12 weeks (toenail). Itraconazole is fungistatic against dermatophytes, nondermatophyte mold and yeasts. Effective schedules include "pulse dosing" at 400 mg daily for 1 week per month or continuous dose of 200 mg daily, both of which require 2 months of treatment for fingernails and 3 months for toenails.
Early in the HIV epidemic, it was clear that pruritus was a marker of HIV infection. Many cases have been labeled as "pruritic papular eruption" which is not a specific disease entity. It encompasses many forms of HIV-associated pruritus. Algorithm 21(A) illustrates one of the clinical approaches to HIV-associated pruritus.
Eosinophilic folliculitis is the most common pruritic follicular eruption that mainly affects adult HIV-infected men having sex with men. Nevertheless, it has also been reported in male injection drug users and women. This condition is characterised by erythematous papulopustules that predisposes to the trunk with occasional involvement on the face and neck. As chronic intense pruritus is the rule, patients often present with heavily excoriated lesion or secondary prurigo nodularis. Histologic examination shows a mixed inflammatory infiltrate with a predominance of eosinophils and lymphocytes surrounding and invading the follicular and sebaceous epithelia, resulting in destruction of sebaceous gland. Treatment of patients with EF is challenging. Various treatments have been tried. These included oral antihistamines, antimicrobials (metronidazole, itraconazole and permethrin), isotretinoin and phototherapy. Clinical responses are variable and relapses are common once the treatment is discontinued. Potent topical steroid have also been tried with some success, but are associated with skin atrophy on facial lesions and hypopigmentation in dark phototype individual. Recently, 0.1% topical tacrolimus have been suggested to be a valuable alternative to topical steroid.14 The most significant benefit is the relief of pruritus that often occurs within the first month of treatment. However, it takes 1-5 months to clear the folliculitis and requires a satisfactory control of HIV viraemia in order to maintain the remission.
Pennys NS. Skin manifestations of AIDS. London: Martin Dunitz,1995.
Ho KM, Wong KH. Dermatologic manifestations in HIV disease. In Chan KCW, Wong KH, Lee SS, editors. HIV Manual 2001, pp231-245.
Raju PV, Rao GR, Ramani TV, Vandana S. Skin disease: clinical indicator of immune status in human immunodeficiency virus (HIV) infection. Int J Dermatol 2005;44:646-9.
Chen TM, Cockerell CJ. Cutaneous Manifestations of HIV infection and HIV-related Disorder. In: Bolognia JL, Jorizzo JL, Rapini R, editor. Dermatology. Volume 1. Mosby 2003. Chapter 78.
Ward HA, Russo GG, Shrum J. Cutaneous manifestations of antiretroviral therapy. J Am Acad Dermatol 2002;46:284-93.
Kong HH, Myers SA. Cutaneous effects of highly active antiretroviral therapy in HIV-infected patients. Dermatol Ther 2005;18:58-66.
Jung AC, Paauw DS. Diagnosing HIV-related disease: using the CD4 count as a guide. J Gen Intern Med 1998;13:131-6.
Breuer-McHam J, Marshall G, Adu-Oppong A, et al. Alterations in HIV expression in AIDS patients with psoriasis or pruritus treated with phototherapy. J Am Acad Dermatol 1999;40:48-60.
Bartlett JG, Gallant JE. Medical Management of HIV Infection 2004.
Ungpakorn R. Cutaneous manifestations of Penicillium marneffei infection. Curr Opin Infect Dis 2000;13:129-34.
Weinberg JM, Mysliwiec A, Turiansky GW, Redfield R, James WD. Viral folliculitis. Atypical presentations of herpes simplex, herpes zoster, and molluscum contagiosum. Arch Dermatol 1997;133:983-6.
Hengge UR, Tietze G. Successful treatment of recalcitrant condyloma with topical cidofovir. Sex Transm Infect 2000;76:143.
Dauden E, Fernandez-Buezo G, Fraga J, Cardenoso L, Garcia-Diez A. Mucocutaneous presence of cytomegalovirus associated with human immunodeficiency virus infection: discussion regarding its pathogenetic role. Arch Dermatol 2001;137:443-8.
Toutous-Trellu L, Abraham S, Pechere M, et al. Topical tacrolimus for effective treatment of eosinophilic folliculitis associated with human immunodeficiency virus infection. Arch Dermatol 2005;141:1203-8.