Kenny CW CHAN
Mycobacterium avium complex (MAC) is composed of two species, M. avium and M. intracellulare. They are environmental saprophytes found in soil, water and food, including pasteurised milk. MAC causes four diseases in humans:
(a) Disseminated MAC (dMAC) occurs almost exclusively in AIDS. It is characterised by bacteraemia, intracellular infection of numerous other tissues and a high total bacterial burden. The vast majority of infections is caused by M. avium.
(b) MAC-associated immune reconstitution diseases (IRD) was described as early as the era of zidovudine monotherapy. The use of highly active antiretroviral therapy (HAART) has been associated with a dramatic increase in its incidence. HAART-induced virologic suppression and immunologic improvement restore immunity to mycobacterial antigens and result in aggravation of existing disease or unmasking of subclinical infection. Localised lymphadenitis, sometimes with caseous discharge, is the most commonly described manifestation.
(c) Pulmonary MAC may occur in immunocompetent individuals with underlying lung disease. In HIV disease, MAC pneumonitis is unusual, except in the context of IRD.
(d) MAC cervical lymphadenitis occurs in the immunocompetent child from 1 to 5 years of age. MAC has overtaken M. scrofulaceum as the most common cause of scrofula. It is hypothesised that milk serves as the vehicle of transmission.
Acquisition of MAC by an HIV-infected patient is most commonly by ingestion, followed by inhalation, after which a steady increase in the total bacterial burden occurs. Colonisation leads to local infection and then disseminated infection when blood culture frequently turns positive. It is thought that, by inhibition of the fusion of phagosome with lysozome, the bacteria survive within phagocytes which also provide transport for dissemination. One major route of dissemination is via the invasion of Peyer's patches in the gastrointestinal tract, from which dissemination occurs to the mesenteric lymph nodes and then the reticuloendothelial organs of liver, spleen and bone marrow. It is important to make a distinction between colonisation of the respiratory and GI tracts, which requires no specific treatment, and true infection. Disseminated MAC is an independent predictor of mortality.
dMAC occurs mainly with advanced immune suppression and often as a subsequent AIDS-defining illness to another primary opportunistic infection, such as Pneumocystis jiroveci pneumonia (PCP) that occurs with a relatively high CD4 count. dMAC has to be excluded whenever a patient with a CD4 count <100/μL presents with fever, night sweats, diarrhoea, and/or weight loss. Patients often have intra-abdominal lymphadenopathy, hepatosplenomegaly, anaemia and highly elevated alkaline phosphatase. Diagnosis is aggressively pursued by obtaining and culturing blood, bone marrow, lymph node aspirate, liver or spleen tissues, followed by DNA probe. The use of liquid media, such as the BACTEC system, is essential for a rapid diagnosis.
AFB in a sputum smear and/or positive mycobacterial sputum culture is not uncommon in advanced AIDS. Although it may represent colonisation, it is important to rule out pulmonary tuberculosis. MAC pneumonitis is rare unless the patient has recently been started on HAART. Speciation by DNA probe should be performed expeditiously. Similarly, MAC may be recovered from stool. Correlation should be made with clinical presentation and results of cultures from other sites. Symptoms such as diarrhoea and GI bleeding are indications for endoscopy. Indiscriminate treatment based on culture results alone may cause not only unnecessary drug interactions, but resistance which is difficult to overcome when true infection develops.
There are multiple synonyms for the disease, including immune reconstitution disease (IRD), immune restoration syndrome/disease, immune restitution disease/syndrome and immune reconstitution inflammatory syndrome. It is defined as the presentation of clinical deterioration of opportunistic infections in HIV infected patients as a direct result of the enhancement of immune responses to these pathogens during HAART'.1 Because of varied manifestations, a high index of suspicion is required for diagnosis. Mycobacterial diseases are the most common cause of IRD. In contrast to tuberculosis, MAC-associated IRD more often presents as new onset disease rather than aggravation of known disease. Other than MAC and TB, IRD to leprosy, M. kansasii, M. genavense, M. scrofulaceum, M. xenopi and BCG has been described. Features typical of MAC-associated IRD are new onset fever and localised lymphadenopathy (about 70%), after a median of 4 weeks of HAART. Lymphadenopathy presents in the thorax, abdomen or peripherally in roughly equal proportions. Respiratory disease (about 20%) is next in frequency.2 Involvement of the spine, joints, prostate, skin, brain and eye is relatively rare. In IRD, CD4 count might not have increased, but almost invariably there is significant decline of viral load.
The major differential diagnosis is from treatment failure and new opportunistic infections. This is important as treatment approach will be different. Factors to consider are:3
(a) Temporal association between starting HAART and development of clinical phenomena (majority within 3 months)
(b) Unusual clinical manifestations
(c) Unexpected clinical course
(d) Exclusion of alternative explanations e.g. drug resistance, non-compliance with treatment
(e) Evidence of preceding immune reconstitution - e.g. rise in CD4 count, restoration of cutaneous hypersensitivity to MAC Ag, and increased in vitro T cell proliferative response to MAC antigen
(f) Histopathologic or cytologic appearance of unexpectedly florid cell-mediated immune response - e.g. granuloma formation
(g) Preceding fall in plasma viral load, providing evidence of a response to HAART.
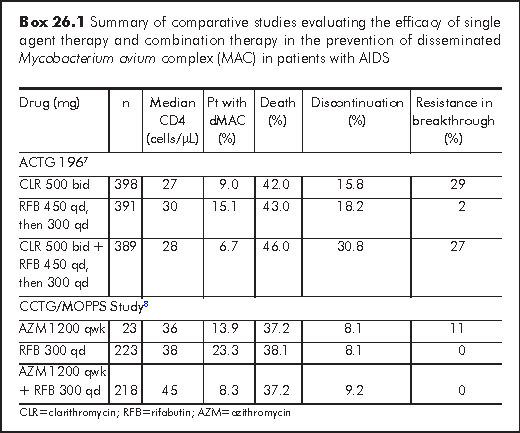
As the organisms are ubiquitous, avoidance of exposure is not practical as a prophylactic measure. On the other hand, chemoprophylaxis is effective. Rifabutin (RFB) 300 mg qd was the first regimen shown to reduce the incidence of disseminated MAC infection.2 Subsequent studies also established the efficacy of clarithromycin (CLR) 500 mg bid3 and azithromycin (AZM) 1200 mg per week.4 In most of these studies, there was survival benefit as well as reduction in disease. Head to head comparisons favoured CLR over RFB and showed no advantage with combination of the two,5 as it was not well tolerated (8.5% developed uveitis) and there was no difference in survival. A similar conclusion was drawn when AZM was compared with RFB (Box 26.1).6

Either weekly AZM or twice daily CLR is well suited for prophylaxis. RFB is best reserved for second line use when the other two drugs are contraindicated or poorly tolerated. The relative merits of the three agents are tabulated in Box 26.2. AZM is probably preferred to CLR for its convenience, lower cost and fewer interactions with concomitant antiretroviral therapy. The lower dosage of 1000 mg per week has been used in Hong Kong with few breakthrough infections (personal communication).
Prior to initiation of chemoprophylaxis, a clinical examination and preferably a blood culture taken for mycobacteria is advisable to rule out subclinical MAC infection. This is an important clinical consideration that is often overlooked when a macrolide is prescribed, leading to the inadvertent development of resistance to this single most important agent against MAC. If RFB is to be used, tuberculosis should similarly be ruled out as there is extensive cross resistance between rifampin and RFB.
If HAART is being started, it is reasonable to withhold primary prophylaxis.9 This allows time for unmasking of subclinical MAC infection when MAC treatment rather than prophylaxis is appropriate. Furthermore, HAART alone leads to a significantly reduced incidence of disease.10 A disadvantage of routine prophylaxis is the emergence of resistance in breakthrough infections. Resistance is more common when prophylaxis was started at a low CD4 count below 20/μL11 and with breakthrough from CLR, the most potent anti-MAC agent. The paradox arises because infection may occur only after resistance to a potent agent has developed. Breakthroughs from AZM and RFB are less likely to be resistant.
Prior to the availability of macrolides and HAART, treatment of dMAC was invariably futile. Success was measured in terms of symptom relief rather than bacteriologic cure. Today, CLR or AZM is used effectively with ethambutol (EMB), especially in the presence of HAART-induced immune recovery.
Macrolide - CLR monotherapy significantly reduces levels of MAC bacteraemia and has led to clinical improvement at a dose of 500 mg twice daily. However, 46% eventually developed in vitro resistance that was associated with a recrudescence of clinical symptoms and increase in bacteraemia. Higher doses cause significant gastrointestinal side effects and higher mortality. Similarly, AZM (500-600 mg once daily) is effective in reducing MAC bacteraemia. In a head-to-head comparison with CLR, AZM was inferior (both drugs used in combination with EMB).12
RFB (bactericidal) and EMB (bacteristatic) are also active against MAC. When they are combined with a macrolide for treatment, it is not only clinically effective,13 but the risk of resistance is reduced.14,15 ACTG 22316 compared three treatment regimens for disseminated MAC: CLR + EMB, CLR + RFB, and CLR + EMB + RFB. It was shown that the 3-drug treatment had better clinical and bacteriologic outcomes, there being more bacteriologic clearance, increased patient survival and less resistance to CLR. By inference, the combination of RFB + AZM + EMB should also be useful, especially as RFB does not reduce AZM levels as it does on CLR. Nevertheless, any increased efficacy of a 3-drug regimen should be balanced against their relative intolerability.
The role of resistance testing in designing an effective MAC treatment regimen is limited to that for macrolides, where resistance is associated with poor outcome. Resistance to other agents is less well studied. Overall, clinical history and progress remain the best guide to a physician treating disseminated MAC infection.
In a patient without prior chemoprophylaxis, the current standard treatment of dMAC is CLR 500 mg bid (AZM 500-600 mg qd is an alternative) and EMB 15 mg/kg qd. If the CD4 count is below 50/μL, and there is no contraindication, it is reasonable to add RFB 300-450 mg qd. In principle, treatment is life long.
In the event that infection breaks through primary prophylaxis, a thorough assessment has to be made regarding adherence, drug malabsorption and possible drug resistance. If available, resistance testing to macrolide is useful.
(a) Breakthrough with RFB prophylaxis - A macrolide and EMB should be used. RFB may be continued.
(b) Breakthrough with AZM prophylaxis - RFB and CLR should be used if no resistance is evident. If not, at least two drugs out of RFB, EMB, amikacin, and a quinolone should be used.
(c) Breakthrough with CLR prophylaxis - If resistance is present, use at least two of the following: RFB, EMB, amikacin, and a quinolone.
Although disease manifestations are different, treatment principles for IRD remain the same in dMAC. In the presence of immune recovery, treatment is usually successful. However, successful symptomatic control may require non-steroidal anti-inflammatory agents, and sometimes systemic steroid of prednisone 1-2 mg/kg/day. In rare instances of life-threatening IRD, such as airway compression by paratracheal lymph nodes or cerebral involvement, surgical intervention and withdrawal of HAART are necessary.
Clinical improvement is anticipated within 4 to 6 weeks, which correlates with a decrease in mycobacteraemia. Sterilisation of blood cultures may take up to 12 weeks. In the presence of a good clinical response, regular monitoring of blood cultures is not obligatory. In contrast, if no response is evident after 4 to 8 weeks, the patient should be reevaluated.
By reason of a high bacterial load, MAC rapidly acquires resistance when treated with single drugs. Active disease therefore has to be treated with at least two active drugs at all times. When a regimen is failing, at least two new drugs must be added or substituted. A salvage regimen is designed from a limited armamentarium after a case-by-case evaluation. Amikacin, a quinolone (levofloxacin, ciprofloxacin or moxifloxacin), or linezolid may be considered. Clofazimine should not be used at all to treat MAC as it was associated with reduced survival.17 The role of resistance testing to drugs other than macrolides is unclear in designing salvage treatment.
Although HAART may unmask subclinical MAC infection in the initial months, overall the incidence of MAC is reduced. HAART is indicated in all patients who have developed opportunistic infections as a result of HIV-associated immune deficiency. Current treatment guidelines also recommend HAART in asymptomatic patients with a CD4 count between 200 and 350/μL.18
Drug interactions - Interactions with rifamycins are important considerations in initiating HAART in a patient concurrently being treated for MAC. For those who are already on HAART when MAC is diagnosed, re-evaluation is necessary. For example, RFB is not "compatible" with the hard gel formulation of saquinavir (unless boosted by ritonavir), and delavirdine (not available in Hong Kong). Dose adjustment is indicated when combined with all protease inhibitors and non-nucleoside reverse transcriptase inhibitors (Box 26.3).19
There is also pharmacokinetic interaction between macrolides and antiretrovirals. In general, standard doses may be used but it is important to look out for untoward reactions. Plasma drug monitoring may be considered in complicated cases.

Evidence is convincing that discontinuation of primary MAC prophylaxis is safe upon good response to HAART, e.g. after CD4 count reaches and stabilises above 100/μL for more than 3 months, especially in the presence of an undetectable viral load. However, it should be re-introduced if CD4 count decreases again to below 50/μL.20
Prior to the era of HAART, patients with disseminated MAC received life-long maintenance therapy. Yet, it is now clear that HAART favourably affects clinical course and discontinuation is possible. The risk of MAC recurrence is small after 12 months of MAC treatment if HAART has led to a sustained response of CD4 to >100/μL for at least six months, and patient is asymptomatic of MAC disease. It is now considered safe to discontinue secondary prophylaxis in such patients but to reintroduce if CD4 falls below 100/μL.
Lawn SD, Bekker LG, Miller RF. Immune reconstitution disease associated with mycobacterial infections in HIV-infected individuals receiving antiretrovirals. Lancet Infect Dis 2005;5:361-73.
Nightingale SD, Cameron DW, Gordin FM, et al. Two controlled trials of rifabutin prophylaxis against Mycobacterium avium complex infection in AIDS. N Engl J Med 1993;329:828-33.
Pierce M, Crampton S, Henry D, et al. A randomized trial of clarithromycin as prophylaxis against disseminated Mycobacterium avium complex infection in patients with advanced acquired immunodeficiency syndrome. N Engl J Med 1996;335:384-91.
Oldfield EC 3rd, Fessel WJ, Dunne MW, et al. Once weekly azithromycin therapy for prevention of Mycobacterium avium complex infection in patients with AIDS: a randomized, double-blind, placebo-controlled multicenter trial. Clin Infect Dis 1998;26:611-9.
Benson CA, Williams PL, Cohn DL, et al. Clarithromycin or rifabutin alone or in combination for primary prophylaxis of Mycobacterium avium complex disease in patients with AIDS: A randomized, double-blind, placebo-controlled trial. The AIDS Clinical Trials Group 196/Terry Beirn Community Programs for Clinical Research on AIDS 009 Protocol Team. J Infect Dis 2000;181:1289-97.
Havlir DV, Dube MP, Sattler FR, et al. Prophylaxis against disseminated Mycobacterium avium complex with weekly azithromycin, daily rifabutin, or both. California Collaborative Treatment Group. N Engl J Med 1996;335:392-8.
Dunne MW, Bozzette S, McCutchan JA, et al. Efficacy of azithromycin in prevention of Pneumocystis carinii pneumonia: a randomised trial. California Collaborative Treatment Group. Lancet 1999;354:891-5.
Fichtenbaum CJ, Zackin R, Feinberg J, Benson C, Griffiths JK; AIDS Clinical Trials Group New Works Concept Sheet Team 064. Rifabutin but not clarithromycin prevents cryptosporidiosis in persons with advanced HIV infection. AIDS 2000;14:2889-93.
Lange CG, Woolley IJ, Brodt RH. Disseminated mycobacterium avium-intracellulare complex (MAC) infection in the era of effective antiretroviral therapy: is prophylaxis still indicated? Drugs 2004;64:679-92.
Baril L, Jouan M, Agher R, et al. Impact of highly active antiretroviral therapy on onset of Mycobacterium avium complex infection and cytomegalovirus disease in patients with AIDS. AIDS 2000;14:2593-6.
Craft JC, Notario GF, Grosset JH, Heifets LB. Clarithromycin resistance and susceptibility patterns of Mycobacterium avium strains isolated during prophylaxis for disseminated infection in patients with AIDS. Clin Infect Dis 1998;27:807-12.
Ward TT, Rimland D, Kauffman C, Huycke M, Evans TG, Heifets L. Randomized, open-label trial of azithromycin plus ethambutol vs. clarithromycin plus ethambutol as therapy for Mycobacterium avium complex bacteremia in patients with human immunodeficiency virus infection. Veterans Affairs HIV Research Consortium. Clin Infect Dis 1998;27:1278-85.
Chaisson RE, Keiser P, Pierce M, et al. Clarithromycin and ethambutol with or without clofazimine for the treatment of bacteremic Mycobacterium avium complex disease in patients with HIV infection. AIDS 1997;11:311-7.
Dube MP, Sattler FR, Torriani FJ, et al. A randomized evaluation of ethambutol for prevention of relapse and drug resistance during treatment of Mycobacterium avium complex bacteremia with clarithromycin-based combination therapy. California Collaborative Treatment Group. J Infect Dis 1997;176:1225-32.
Gordin FM, Sullam PM, Shafran SD, et al. A randomized, placebo-controlled study of rifabutin added to a regimen of clarithromycin and ethambutol for treatment of disseminated infection with Mycobacterium avium complex. Clin Infect Dis 1999;28:1080-5.
Benson CA, Williams PL, Currier JS, et al. A prospective, randomized trial examining the efficacy and safety of clarithromycin in combination with ethambutol, rifabutin, or both for the treatment of disseminated Mycobacterium avium complex disease in persons with acquired immunodeficiency syndrome. Clin Infect Dis 2003;37:1234-43.
Shafran SD, Singer J, Zarowny DP, et al. A comparison of two regimens for the treatment of Mycobacterium avium complex bacteremia in AIDS: rifabutin, ethambutol, and clarithromycin versus rifampin, ethambutol, clofazimine, and ciprofloxacin. Canadian HIV Trials Network Protocol 010 Study Group. N Engl J Med 1996;335:377-83.
DHHS Panel on antiretroviral Guidelines for Adults and Adolescents - a Working Group of the Office of AIDS Research Advisory Council. Guidelines for the use of antiretroviral agents in HIV-1 infected adults and adolescents, May 4, 2006. Available from http://AIDSinfo.nih.gov (accessed Jun 14, 2006).
US CDC. Division of Tuberculosis Elimination. TB/HIV drug interactions. Available from http://www.cdc.gov/nchstp/tb/TB_HIV_Drugs/TOC.htm (accessed Jun 14, 2006)
Kaplan JE, Masur H, Holmes KK; USPHS; Infectious Disease Society of America. Guidelines for preventing opportunistic infections among HIV-infected persons--2002. Recommendations of the U.S. Public Health Service and the Infectious Diseases Society of America. MMWR Recomm Rep 2002;51(RR-8):1-52.